Vitamine K2 mk7
(link Orthokennis)
Vitamine K2 mk7 net zo belangrijk voor
calcium transport
Vitamine K2 mk7 blijkt een uitzonderlijk goed middel tegen
aderverkalking maar kan zelfs al, zoals bij vele oudere mensen,
aanwezige aderverkalking geheel ongedaan maken. Bij een goed
darmflora wordt door de darmbacterien per dag zo'n 100 ug
gemaakt en in het lichaam ogenomen en bij een tekort is dat ook
een goede hoeveelheid om als supplement te nemen maar voor het
herstel van de verkalkte aderen is 360 ug aangeraden per dag.
Met een aderdichtslibbingfactor van 15% kan dit al na 1 maand
hersteld zijn. Bij 30% na 4 maanden en 60% na 10 maanden 360 mg
vitanine k2 mk7. En ook de elasticiteit hersteld weer geheel.
Ook blijkt het uitstekend te werken tegen osteoporose
https://www.youtube.com/watch?v=0Hgsy46UqsA
http://www.praktijklijnen.nl/wp-content/uploads/2017/08/Vitamine-K2-meten.pdf
Video
Vitamine D
vitamindhealth.org
Vitamine D veel belangrijker dan gedacht ook
voor CVS ME
Vitamine D blijkt veel belangrijker voor de
gezondheid dan gedacht. Het is bij heel veel processen in het
lichaam betrokken en tekort vitamine D in het bloed komt veel
voor bij CVS ME.
Twintig tot dertig minuten in de zon maakt 10.000 iu ofwel 250
µg vitamine D aan.
Behalve als je een zeer donkere huid hebt dan is daarvoor een
uur noodzakelijk.
Twee tot drie maal per week 15 - 20 minuten met blote armen of benen als de zon
hoog staat is optimaal voor de aanmaak van Vitamine D en tegelijkertijd ook
noodzakelijk. Deste hoger de zon staat deste meer UVB er in het zonlicht zit en
deste meer aanmaak vit D, voor 10.00 uur en na 15.00 uur is er geen
aanmaak. In april tot en met september geeft zonlicht een zeer goede hoeveelheid vitamine
D. In de winter (in Nederland van Oktober tot en met Maart) wordt geen vitamine D gemaakt door zonlicht omdat er dan geen
UVB in
het zonlicht zit. Dan neemt men om een goede gezondheid te behouden minimaal 1000 iu (25 µg)
D2 of D3 per dag. Optimaler 5000 iu 125 µg per 3 dagen of 2000 tot 4000 iu 50 - 100 µg per dag.
Dit zijn indicaties van op dit moment door vitamine D
onderzoekers aanbevolen hoeveelheden. Veel hoger dan de ADH.
Volgens het NIH in de US is 2000 iu per dag zeker veilig.
Vitamine D activeerd
je immuunsysteem het
activeert peptides
die virussen en
bacteria doden.
video
Het zorgt
ervoor dat je tot
90% minder gevoelig bent
voor virussen en
bacteria
Het is ook heel
belangrijk voor de
tanden. En beter dan
fluor.
Vitamin D3 is goed en Vitamine D2 is bijna net
zo goed. De combinatie is ook net zo goed maar ook niet beter dan D3 of D2.
Vitamine D is een hormoon.
Met zonlicht worden verschillende soorten vitamine D (D1 t/m D5) en andere
fotoproducten gemaakt waarvan de werking
nog onderzocht moet worden en is dus wel anders dan vitamine D inname.
Zonnebank is ook goed voor de aanmaak van vitamine D liefst wel een
zonnebank met meer
uvB dan de gemiddelde.
Per 100 iu (2.5 µg) Vitamine D inname per dag stijgt
bloedhoeveelheid met 1 µg/L
30 µg/L is het echte minimum. Van 30 tot 50 µg/L is te laag. Vanaf 50 µg/L is goed. 60 tot 80 µg/L is optimaal.
Bij een bloedwaarde tussen de 30 en 50 µg/L is een supplement nodig.
Bij waarden beneden de 30 µg/L is een supplement noodzakelijk.
Video
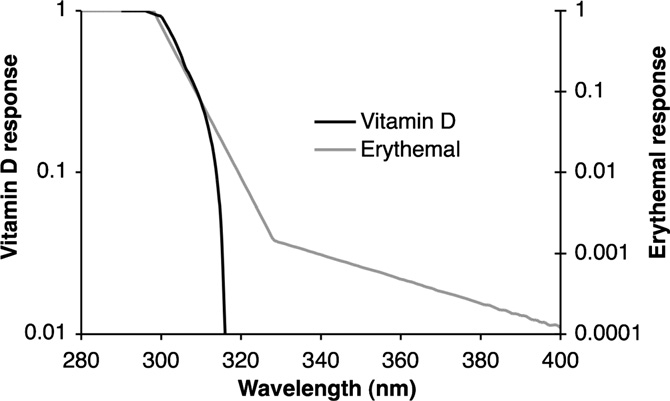
UVB 280-315nm UVA 315-400nm Vitamine D aanmaak 270-315nm. Boven 300nm steile
afval.
Kan men met voldoende vitamine D, opgedaan in de zomer, de winter doorkomen?
Nee het lichaam kan een beperkte hoeveelheid opslaan en dit raakt op na twee
weken als er niets binnenkomt zoals in de wintermaanden.
Vitamine D tekort heeft een verband met:
Autoimmuun-ziekten, multiple sclerose, osteoporose, fybromyalgia, hart en vaat
ziekten, darm~, borst~ en prostaatkanker, diabetes type I, rachitis,
osteomalacie, myopathie, depressie, chronische pijn, migraine, schizofrenie,
hoge bloeddruk, reumatoïde artritis, verhoogd cholesterol niveau.
50% van de wereld bevolking heeft vitamine D tekort.
Kleding houdt UVB tegen.
Zonnebrand creme houdt UVB tegen en voorkomt de aanmaak van vitamine D.
Een donkere huidskleur of een aanleg voor een donker huidskleur houdt UVB
gedeeltelijk tegen en zorgt voor een sneller ontstaan van vitamine D tekort.
De menselijke huid maakt onder invloed van zonlicht ook fumaarzuur aan.
Fumaarzuur ofwel fumarate is een stof die ook noodzakelijk is in de
mitochondrien voor atp productie.
Vitamin D and backpain
The report, "Vitamin D A Neglected 'Analgesic' for Chronic Musculoskeletal
Pain," which was peer-reviewed by a panel of 8 experts, includes the following
important points:
-- Vitamin D is essential for
calcium absorption and bone health. Inadequate vitamin D intake can result
in a softening of bone surfaces, or osteomalacia, that causes pain. The lower
back seems to be particularly vulnerable to this effect.
-- In one study of 360 patients with back pain, all of them were found to have
inadequate levels of vitamin D. After taking vitamin D supplements for 3 months,
symptoms were improved in 95% of the patients. All of them with the most severe
vitamin D deficiencies experienced back-pain relief.
-- The currently recommended adequate intake of vitamin D up to 600 IU per day
is outdated and too low. According to the research, most children and adults
need at least 1000 IU per day, and persons with chronic back pain would benefit
from 2000 IU or more per day of supplemental vitamin D3 (also called
cholecalciferol).
-- Vitamin D supplements have a highly favorable safety profile. They interact
with very few drugs or other agents, and are usually not harmful unless
extremely high doses such as 50,000 IU or more are taken daily for an extended
period of time.
Vitamin D deficiency
In some people, the problem might not be
enough magnesium, but instead might be not enough vitamin D, which has an
effect on magnesium absorption. Up until recently, doctors only associated
a vitamin D deficiency with weak bones, and they believed that a vitamin D
deficiency in young people was rare in countries like the US. However, both
of these beliefs have been proven false. Not only does it occur in young
people, but sometimes a vitamin D deficiency
can manifest
itself mainly as pain.
Initial symptoms in adults can often appear as vague musculoskeletal pains,
muscle weakness, and fatigue, symptoms commonly found in fibromyalgia.
Also, studies on the muscles of vitamin D deficient
patients,
show a reduction
of ATP levels, similar to that of fibromyalgia patients.
In some cases, the deficiency leads to
myopathy, with quite severe muscle weakness, especially affecting the legs
and ability to walk. On the other hand, sometimes the symptoms are less
severe, in which case it could be easily overlooked in fibromyalgia
patients. In fact, several small studies have shown that at least 40% of
patients with fibromyalgia have a vitamin D deficiency.vitamin D subnutrition is common in patients with FM
And while some blood tests can possibly indicate a vitamin D deficiency,
often a deficiency can exist without any
other biochemical changes. Thus, the
only definite way to tell if you have this problem,
is by testing vitamin D levels. Unfortunately, very few doctors do this.
So It's quite possible that some people who have
fibromyalgia, might also have a vitamin D deficiency. Or perhaps they never
had fibromyalgia to begin with. In the following study from Canada, only
12% of patients referred to rheumatologists with the diagnosis of
fibromyalgia, actually had fibromyalgia:
Vitamin D deficiency is often
misdiagnosed as ME/CFS or fibromyalgia as the
major symptoms include muscle pain and weakness,
according to Michael F. Holick, MD, PhD, of the
Boston University School of Medicine. Other
researchers (Shinchuk & Holick) agree saying
that all patients presenting with symptoms
suggestive of ME/CFS should be tested for
vitamin D deficiency.
Some studies have suggested
that over 25% of ME/CFS patients have low vitamin D
levels.
Studies have shown that
vitamin D supplements can significantly reduce pain
with one showing that vitamin D deficient people
require twice as many painkilling drugs.
People getting no sunlight should supplement with at
least 1,000 IU of vitamin D, which is 5 times the
usually recommended amount [Glerup].
Vitamin D is a powerful immune
system modulator with most immune cells having
receptors for the active form of the vitamin. It is
suggested that vitamin D may enhance innate immunity
and inhibit the development of allergies and certain
autoimmune conditions. These actions may be
important for the immune dysfunction in ME/CFS.
Technically not a
"vitamin," vitamin D is in a class
by itself. Its metabolic product,
calcitriol, is
actually a
secosteroid hormone
that targets over 2000 genes (about
10% of the human
genome) in the
human body. Current
research has implicated
vitamin D deficiency as a
major factor in the pathology of at
least 17 varieties of cancer as well
as heart disease, stroke,
hypertension, autoimmune diseases,
diabetes, depression, chronic pain,
osteoarthritis, osteoporosis, muscle
weakness, muscle wasting, birth
defects, periodontal disease, and
more.
Vitamin D's influence on key
biological functions vital to one's
health and well-being mandates that
vitamin D no longer be ignored by
the health care industry nor by
individuals striving to achieve and
maintain a greater state of health.
Sunshine and Your
Health Vitamin D
If well adults and
adolescents
regularly avoid
sunlight exposure,
research
indicates a
necessity to
supplement with at
least 5,000 units (IU)
of vitamin D daily.
To obtain this
amount from milk one
would need to
consume 50 glasses.
With a multivitamin
more than 10 tablets
would be necessary.
Neither is
advisable.
The skin produces
approximately 10,000
IU vitamin D
in response 20–30
minutes summer sun
exposure—50 times
more than the
US
government's
recommendation of
200
IU per day!
Sun exposure
The maximum amount
of vitamin D that is
cutaneously produced
under UV light
stimulation,
creating serum
25(OH)D
concentrations
similar to those
resulting from an
oral dose of 250 µg
OBJECTIVE: To
estimate the amount,
type, and tissue
distribution of
vitamin D in the
adult body under
typical inputs.
METHODS: Review and
reanalysis of
published
measurements and
analysis of tissue
samples from growing
pigs raised in
confinement on diets
providing about 2000
IU vitamin D/day.
Cholecalciferol and
25-hydroxyvitamin D
[25(OH)D]
concentration
measured by HPLC.
RESULTS: Mean serum
25(OH)D in all
studies combined was
45 nmol/L. At the
level of vitamin D
repletion
represented by this
concentration, total
body vitamin D would
be 14,665 IU for a
70 kg adult woman.
65% of this total
was present as
native
cholecalciferol and
35% as 25(OH)D.
Nearly
three-quarters of
the cholecalciferol
was in fat, while
25(OH)D was more
evenly distributed
throughout the body
(20% in muscle, 30%
in serum, 35% in
fat, and 15% in all
other tissues). At
the daily vitamin D
consumption rates in
these animals total
body stores provided
only a approximately
7-day reserve.
CONCLUSIONS: At
total intakes on the
order of 2000 IU/day,
an adult has very
little vitamin D
reserve, despite
intakes 10x the
current
recommendations.
Those recommended
inputs need to be
increased by at
least an order of
magnitude. Food
tables that fail to
take into account
25(OH)D content of
various meat
products lead to
underestimation of
dietary vitamin D
intake.
In a
trial conducted
by Barger-Lux et al,
vitamin D3
doses of
25, 250, and 1250 µg
per day were
administered to 38
healthy men
for 8 wk.
New save DRA 250 µg
per day?
Many vitamin
D-containing dietary
supplements for
adults are
formulated to
provide 5–10 µg/d,
when used according
to the label
instructions.
Although rare and
not widely
available, a few
supplements now
contain as much as
1250 µg vitamin D/d.
Exposure of a person
in a bathing suit to
a minimal erythemal
dose of sunlight,
which is typically
no more than 15-20
minutes on Cape Cod
in June or July at
noon time, is the
equivalent to taking
20,000 IU of vitamin
D orally. It is now
well documented that
in the absence of
any sun exposure
1,000 IU of vitamin
D3 a day is
necessary to
maintain healthy
levels of
25-hydroxyvitamin D
in the circulation.
Vitamin D deficiency
results in chronic
fatigue and
multi-system
symptoms
Vitamin D should be
taken with high dose
Calcium 1200 mg and
in severe cases up
to 2400 mg/day
divided in 4 doses
of 300 to 600 mg.
Author: Dr. med.
Anna Dorothea Hoeck,
MD, Mariawaldstr. 7,
50935 Cologne,
Germany. E-Mail:
ad.hoeck@tonline.
de
No potential
conflicts of
interest exist in
this paper.
Initially, all
metabolic disorders
cause nonspecific
symptoms combined
with fatigue
It was in 1993, when
I detected, that not
only such common
metabolic disorders,
like thyroid
diseases, iron and
vitamin B12
deficiencies, cause
nonspecific symptoms
like chronic fatigue
and functional
disorders, but as
well vitamin D
deficiency (1). Not
only these symptoms
could
be observed in
vitamin D deficiency,
but as well frequent
infections,
allergies and
widespread
intolerances, pains,
sleep disorder, mood
and personality
changes (1,2).
In these early days,
I found out an
optimal treatment
dose of 5,000 –
10,000 IU (125-250
mcg) cholecalciferol
by dose-response
trials (2).
Initially, I
hesitated to combine
such high
doses with calcium,
because of potential
hypercalcemia and
hypercalciuria. But
addition of a
base powder,
containing
multi-minerals, and
calcium as well,
seemed to optimize
treatment
results (2).
The striking
resemblance between
the symptoms of
vitamin D deficiency
and chronic fatigue
syndrome (CFS/ME),
as well as the low
levels of the
meanwhile accepted
biomarker for
vitamin D deficiency,
25-hydroxyvitamin D
3, which is named as
well 25-
hydroxycholecalciferol
(25OHD3), induced me
to treat CFS/ME
patients with
cholecalciferol
(vitamin D3).
However, though
patients with mere
chronic fatigue
recovered soon, most
with
full-blown CFS/ME
did not respond
remarkably to
treatment. In
particular patients
with
calcium serum levels
near the lowest or
highest normal range
seemed to be the
most vitamin
D resistant (2).
When I realized that
combination with
calcium is mandatory
for treatment
response, I
substituted with 500
to 1,000 mg
elementary calcium
per day, which might
have been, in
retrospective view,
a perhaps too low
dose for assumed
severe calcium
deficiency following
chronic vitamin D
deficiency (3-10).
2
Vitamin D deficiency
is a hidden disorder
of high frequency
Vitamin D deficiency
is by no means rare
(3,11-15). In
particular, highly
gifted and engaged
people working most
of time indoors, but
as well poor and
socially deprived
people are at
high risk, due to
their common problem,
the lack of sunlight.
Vitamin D
insufficiency,
showing 25OHD3
levels from 20-30 ng/ml
(50-80 nmol/L) even
in
summer time, is
quite common, but
already entailing
the threat of
chronic depletion of
body
calcium stores, and
chronic infections
(11-14). Levels from
10-20 ng/ml (25-50
nmol/L) are
measured frequently
in winter season.
This aggravates
calcium deficiency
substantially.
Severe vitamin D
deficiency with
levels below 10 ng/ml
(25 nmol/L) causes
severe fatigue
and personality
changes,
depression-like
symptoms, chronic
sleep disorder,
multiple
intolerances,
obvious immune
dysfunctions and in
the long time,
multi-system
symptoms and
multi-system
diseases (1,2).
Vitamin D deficiency
leads inevitably to
calcium and other
mineral deficiencies
Long lasting or
chronically repeated
25OHD3 levels
beneath 30 ng/ml
(80nmol/L) result in
compromised calcium
absorption in the
bowel, and
inefficient fixation
of calcium and
phosphate, as well
as all other
minerals, stored in
bone (4-10). This
means, chronic
vitamin D
deficiency can not
be separated from
the clinical
consequences of
calcium and
phosphate, and
overall mineral and
base deficiency
(11-15).
Due to lowered body
stores of calcium, a
special “calcium
rescue-hormone”,
synthesized in
little glands (parathyroidea)
positioned very
closely (“para”) to
the thyroid,
augments its
production and
secretion. This
hormone is called
parathormone (PTH)
(5,7,8,10).
PTH enhances calcium
absorption in the
bowel and tubular
calcium “re-uptake”
(reabsorption)
in the kidney (5,7).
Thus PTH helps to
compensate for net
calcium deficiency.
However, PTH
mobilizes as well
bone calcium stores
thus acting as a
so-called
“osteolytic”
hormone (5,7). That
means, at the costs
of bone calcium, PTH
tries to normalize
appropriate
serum levels of
calcium which are
mandatory for proper
neural and general
cellular function
(5,7,8,10,14).
If enough stores of
25OHD3 and calcium
circulate in blood,
PTH levels are
undulating with
peaks and troughs.
In case of low
stores, in contrast,
PTH will be
constantly elevated.
As PTH
enhances the
conversion from the
pro-hormone 25OHD3
to the more
metabolically active
hormone
1,25-dihydroxycholecalciferol
[1,25(OH)2D3]
(5,7,8), the latter
will also be
constantly elevated,
as long as any
25OHD3 will be
available. Due to
the high conversion
3
rate, 25OHD3 stores
become depleted more
quickly. Moreover,
depleted stores
compromise
a constant rate of
conversion. It is
important to realize
that a persistent
elevation of PTH and
low stores of 25OHD3
are no healthy
conditions, and
disturb profoundly
cell functions and
metabolism. Normally,
1,25(OH)2D3 is
converted only when
the cell needs it.
Furthermore,
persistent elevation
of PTH augments
constantly the
relation of free to
protein-bound
calcium
in the cells (3-15).
This as well is
detrimental for
cells, finally
causing multisystem
diseases
(3-15).
The multiple actions
of vitamin D become
more and more
acknowledged in
research
Besides the
classical and well
known actions on
bone, gut and kidney,
most tissues possess
nuclear vitamin D
receptors
(11,12,15-18,20).
More than 200 genes
are now known to be
influenced by
vitamin D (11,12).
Besides these
actions on gene
expression, it acts
as well on
cell signalling by
multiple mechanisms
(8,15,19,20). Many
common and frequent
diseases,
like heart problems,
diabetes,
hypertension,
Parkinson’s disease,
multiple sclerosis,
and colon,
prostate and breast
cancer, as well as
chronic inflammatory
and autoimmune
diseases, are
now discussed as
co-induced by
vitamin D deficiency
(8,21-34). This
points to the impact
of
vitamin D deficiency
and vitamin D
resistance for the
general population
(8,21-34), and to
the
importance to
substitute vitamin D
and calcium in many
chronic health
problems (21-34).
In particular,
immune system takes
profit from
treatment (22-30).
Vitamin D supports
the
primary (innate)
immune answer
strongly (22-27),
but regulates,
modifies and
mitigates the
secondary (cognate)
immune answer
(22,26-29), and
inhibits the nuclear
factor kappa-B (NFKB)
which is an
important
pro-inflammatory
switch signal in
cells (30), thus
preventing
chronic inflammation
and autoimmunity by
multiple mechanisms
(22-30). Meanwhile,
recent
new research about
immune regulatory
cells elucidates
more clearly the
connection between
chronic fatigue and
chronic inflammation
(35). These insights
fit very well to
already existing
results of vitamin D
research (22).
Chronic fatigue
syndrome, a
condition of vitamin
D resistance?
As sufficient stores
of vitamin D and
calcium are
mandatory for
general health
(8-15),
CFS/ME as a severe
health problem,
accompanied by
immune dysfunctions
and high grade
disability, should
be focussed as well
(11), though not yet
broadly discussed in
literature (3).
In case of chronic
disease,
lifetime-stabilization
of seasonal
fluctuations of
vitamin D level
will enhance calcium
absorption (11,12);
calcium substitution
will restore already
existing
calcium body
deficits
(5,8,11,12), thus
reducing high
turnover of vitamin
D (8,38,39) and
vitamin D resistance
(8,38,39).
4
Vitamin D de- or
insufficiency can be
easily identified by
serum 25OHD3 levels.
However, it
is difficult to
prove chronic
calcium deficiency
by serum
measurements. The
well known
osteolytic actions
of parathormone and
inflammatory
cytokines result in
misleading rise of
serum calcium levels
obscuring the real
whole body calcium
deficits (4-6,14).
Furthermore, it must
be kept in mind that
both calcium
deficits (36) and
high
oxidativenitrosative
stress (37) result
in altered protein
shapes (secondary
structure) which
highly
compromise enzymatic
and other biologic
functions. Both
mechanisms may
substantially
contribute to the
observed vitamin D
resistance of
patients with CFS/ME.
In order to overcome
this resistance,
substitution doses
should be high
enough. 25OHD3
levels should be
higher than 40 ng/ml
(100 nmol/L)
(13,38). As
ergocalciferol is
less potent,
but nevertheless
raises 25OHD3 levels,
cholecalciferol
would be the
preferred compound,
if
locally available
(9). At least 2,000
IE (50 mcg)
cholecalciferol, but
often higher doses
up to
10,000 IE (250 mcg)
per day, are
necessary (38,39).
The daily amount of
calcium should be at
least 1200 mg, given
3-4 times a day, in
divided single doses
between 300 - 600 mg
(5,8).
Calcium needs in
severe diseases are
reported to be as
high as 2400 mg per
day (5,8,10,39).
Last, but not least,
it should be
mentioned that
cholecalciferol as
chemical derivative
of
cholesterol is an
important
antioxidant (40),
and is able to
restore redox
balance (36). Both
actions are supposed
to be of additional
usefulness in CFS/ME.
Summary
Physicians should
realize that chronic
fatigue is not a
primary mental
disease. Vitamin D
deor
insufficiency seems
to be the most
frequent cause. If
untreated, calcium
depletion and
vitamin D resistance,
presumably further
deficiencies, and
for instance,
chronic fatigue
syndrome will
develop, later on
followed by other
more obvious
diseases. Vitamin D
resistance of
chronic fatigue
syndrome should be
treated with much
higher doses of
vitamin D
and calcium, than
applied in
osteoporosis
prophylaxis.
Clinical high
quality studies
would be helpful to
get an overview
which doses of
calcium and
vitamin D will be
optimal and
appropriate in CFS/ME,
and reveal the rate
of treatment
responses. Possibly,
further
micronutrient
co-medications will
be necessary in
severe cases of
CFS/ME.
|
